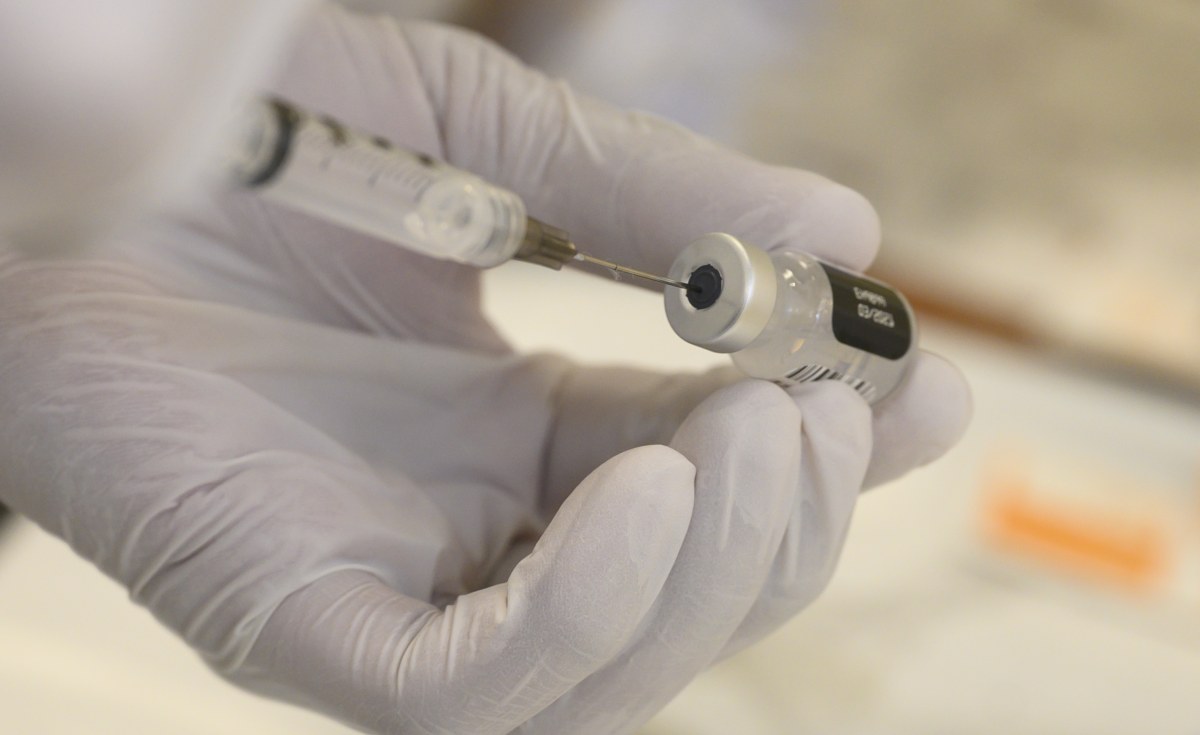
Very few vaccines have found their way into the arms of Africans as they struggle with a surge in COVID-19 infections. Several countries now want to start producing vaccines on the continent. Can they succeed?
The third wave of coronavirus is rolling through much of Africa — and it could be the most severe of the pandemic yet, experts fear. The conditions on the continent could not be worse: The more contagious and arguably more dangerous delta variant of the SARS-CoV-2 virus, which has already wreaked havoc in India, is now spreading in Africa, where it is encountering a largely unvaccinated population.
According to the African Union’s (AU) disease control agency, Africa CDC, just over one percent of the African population has been fully vaccinated, around two and a half percent have received at least the first dose. By comparison, in the EU, at least 50% of the population has now received the first dose, according to “Our World in Data,” and one in three already has full vaccination protection.
“A wake-up call” for Africa
This disparity in the supply of COVID-19 vaccines is causing anger and incomprehension among many African politicians. “The selfishness in this world is bad,” Uganda’s President Yoweri Museveni, for example, said last week at the World Health Summit in Kampala. But he also used his opening speech to warn his African counterparts: The current situation is a wake-up call, Museveni said. “It is a shame that the African continent is sleeping and waiting to be saved by others.”
African countries have so far relied almost entirely on vaccine imports from North America, Europe, and Asia not only in the fight against COVID-19 but also against diseases such as measles, tetanus, and tuberculosis. Only about one percent of all vaccines administered on the continent are produced in Africa, and active production facilities currently exist only in Tunisia, Algeria, South Africa, and Senegal.
That is precisely what is now set to change. Several African countries are currently working to promote the local production of vaccines. The African Union wants to produce 60% of the vaccines needed in Africa by 2040 — and as soon as possible, African vaccines shall also reduce the COVID-19 pandemic.
But why is Africa only now getting into vaccine production? What are the difficulties in setting up the production lines? And how quickly can the plans be implemented at all? The most important questions and answers at a glance:
Why are hardly any vaccines being produced in Africa so far?
Basically, the technical hurdles for the production of vaccines are very high. Not only is the construction of specialized production and filling facilities costly, but the training and further education of qualified personnel require massive investments. Even in highly industrialized countries such as the US or Germany, the development and production of vaccines are therefore supported with gigantic government investments.
Many African governments cannot afford these. It is, therefore, no coincidence that the few existing production facilities in Africa, such as those of the Pasteur Institutes in Senegal, Tunisia, and Algeria, are largely financed by development cooperation. Thus, for example, projects that are less well funded in Nigeria or Ethiopia have not yet succeeded in bringing vaccine production to market maturity, despite years of effort.
What has changed as a result of the pandemic?
Since the beginning of the pandemic, but especially since the start of vaccination campaigns in the Global North, building local vaccine capacities has been high on the agenda of many African countries. Numerous projects are already in the pipeline, ranging from forays by individual companies or countries to establish so-called “regional vaccine hubs” involving several countries. These initiatives are financed and supported by the EU, the World Bank, and other international donors. German Health Minister Jens Spahn also pledged aid of up to €50 million ($59 million) during a visit to South Africa in May.
What exactly do the projects look like, and how quickly can they be implemented?
Most of the announced projects are aimed at the local production or filling of already licensed vaccines in existing production facilities. Since, apart from the licensing negotiations, only the production lines have to be adapted and the raw materials procured, these projects can be realized relatively quickly.
South Africa’s Aspen Pharmacare has been the quickest to respond and is so far the only one on the continent producing a COVID-19 vaccine on behalf of the US company Johnson & Johnson. Egyptian company VACSERA plans to begin manufacturing the Chinese Sinovac vaccine in the coming weeks. Similar cooperation agreements between African pharmaceutical companies and international vaccine manufacturers also exist in several other countries, such as Senegal and Algeria.
Less quick to implement are plans where the appropriate production or filling facilities have yet to be built. It takes around 18 months to set up a fill-and-finish production line, says Simon Agwale, biotech entrepreneur and director of the African Vaccine Manufacturers Alliance (AVMI). And there’s another problem, he says: “Because of the pandemic, there’s a long waiting list right now for manufacturers of such equipment.” As a result, he does not believe that the ambitious timelines of some governments that have announced locally produced vaccines for this year can be met.
Financing such projects is also more complicated and lengthy. “Everyone is talking about building factories for COVID-19 vaccine production right now. But what happens after COVID?” says Agwale. According to him, there needs to be a concrete plan for how, for example, mRNA production facilities needed for BioNTech’s or Moderna’s COVID-19 vaccines could later be used for other vaccines. A technology transfer center for mRNA vaccines is currently being built in South Africa and is not expected to be operational until summer 2022.
Other challenges
The challenges to building a dedicated vaccine infrastructure in Africa are immense. In addition to the usual difficulties such as financing and a lack of technical expertise, issues surrounding patent protection, which have been discussed for many months, have still not been resolved. It is also questionable whether the bulk of the projects currently being pursued in Africa will actually make the continent less dependent on pharmaceutical companies from the developed nations.
According to AVMI Director Simon Agwale, most projects are filling plants that rely on the supply of raw materials by vaccine manufacturers. While this is welcome in principle, he says: “If there is not also investment in the production of the actual substances, we end up with countless filling plants, but no product that can be filled.”